Leaders in Physiotherapy and Physio-led Exercise

EMBRACE
YOUR
INNER
STRENGTH
Welcome to Inner Strength Bayside Physiotherapy
We are a Physiotherapy Clinic based in Cheltenham that offers an effective and personalised approach to treatment that includes Physiotherapy and Physio-led Exercise programs.
Physiotherapy treatment methods include joint mobilisation, massage, dry needling, kinesio and rigid taping and rehabilitation including clinical exercise.
We treat all musculoskeletal conditions including back and neck pain, headaches, pre and post-natal concerns including mastitis (with therapeutic ultrasound) and pelvic floor concerns, sporting injuries and we manage rehabilitation following injury or surgery. We also specialise in Cancer Rehabilitation, with Luci offering the Pinc and Steel Cancer Rehab Programs.
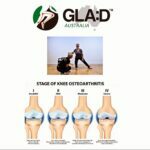
Our physios are also trained in The GLA:D program. The best first treatment for hip and knee osteoarthritis. This program provides exercise and education over six weeks to help you regain your life.
COVID UPDATE: Masks are optional, however, we recommend all patients to wear a mask in the treatment rooms, especially if you have any respiratory symptoms. Please also sanitise your hands on arrival.
Why Inner Strength
- State of the art equipment
- Friendly and experienced team
- Personalized and attentive service
- Modern approach to healthcare
- Motivated to help patients achieve goals
- On the spot health rebates available